Millions of Americans have plantar fasciitis and your risks of developing it double as you get older. Don’t let heel pain hold you back from an active, vibrant life. Learn the causes of plantar fasciitis, plus how to properly treat it naturally and without surgery, so you can get back to doing the things you love.
What Are the Symptoms of Plantar Fasciitis?
There are many reasons why you may be experiencing heel pain, but research shows that plantar fasciitis is the most common cause of heel pain.
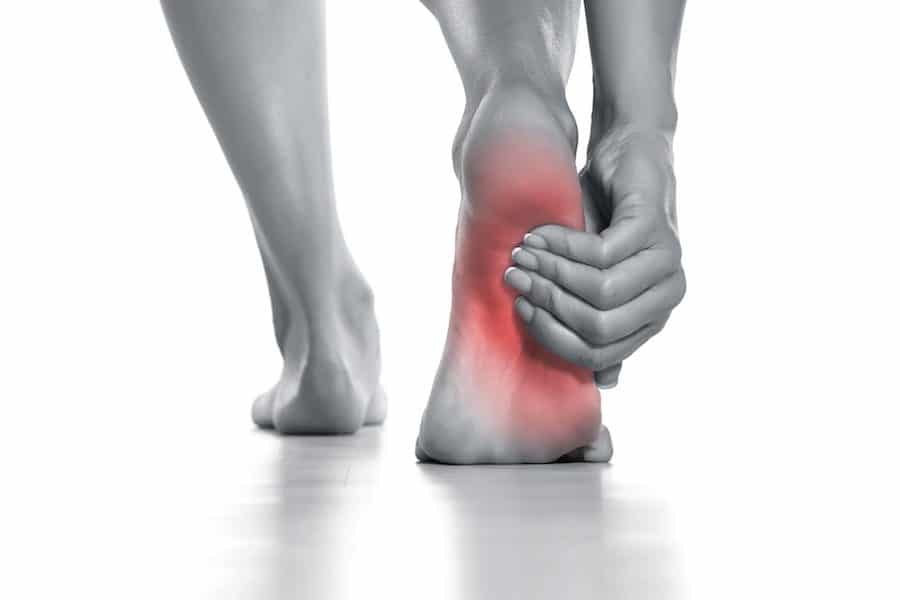
The plantar fascia is a ligament that runs from your heel through your foot. It helps to support your foot’s natural arch when you walk or run. If your heel pain is caused by this very common condition, your symptoms may include:
- Pain at the bottom of your heel
- Pain that’s worse after periods of inactivity (e.g. when you first wake up, or after you’ve been sitting for a while)
- Pain whenever you’re putting excessive pressure on your arch and heel (e.g. walking up a flight of stairs, prolonged walking, jumping, etc.)
Who Is Most at Risk of Developing Plantar Fasciitis?
Anyone can develop heel pain and plantar fasciitis, but it tends to most often affect the following demographics:
- Overweight and pregnant individuals, because the extra body weight puts more pressure on your feet.
- Very active individuals, since physical activity can inflame your tendons and ligaments.
- Older adults, especially those in their 40s and beyond.
That latter point is key as recent studies have found higher rates of heel pain and plantar fasciitis in older adults. Researchers now believe that plantar fasciitis is the result of degeneration of the plantar fascia ligament in your foot. This begs the question: Could regenerative medicine and regenerative therapies provide better, more effective treatment and healing for plantar fasciitis?
Popular Plantar Fasciitis Treatments
Many people treat heel pain with a combination of home remedies and medical interventions. Common ways to manage plantar fasciitis include:
1. Medication
Approximately two-thirds of people who have plantar fasciitis use over-the-counter anti-inflammatory drugs (i.e. NSAIDs), such as aspirin and ibuprofen. These drugs help reduce inflammation and swelling, which may relieve heel pain but come with a list of side effects with long-term use that include upset stomach to increased cardiovascular and kidney disease.
2. Steroid Injections
Corticosteroids, whether taken orally or injected right into your foot, are often suggested to those who have severe heel pain. Unfortunately, steroid injections carry significant side effects, including the risk of heel fat pad necrosis (permanent deformity and pain in the heel), osteoporosis, increased blood sugar, immune system suppression, and weight gain to name a few.
It’s no wonder that in a national survey of orthopedic surgeons, more than 63 percent of them recommended using alternative therapies instead of steroids.
3. Stretching, Night Splints, Custom Orthotics
Night splints and custom orthotics can alleviate the symptoms of plantar fasciitis by alleviating some of the pressure on the fascia and keeping the fascia in a lengthened position. Unfortunately, these are often cumbersome for people and they are often not worn regularly.
One study found that stretching can be just as effective for heel pain and plantar fasciitis as night splints and custom orthotics. Effective stretching routines include:
- Stretching your calves
- Rolling your arch (use a foam roller or, better yet, a water bottle filled with frozen water)
- Stretching your toes back and up, away from the ground
By improving mobility in your feet and lower legs, you help ease tension that may be exacerbating your plantar fasciitis.
4. Diet
Because extra weight can put more pressure on the plantar fascia, diet can be an effective tool to lose weight and lessen the pressure on the feet associated with plantar fasciitis. Generalized inflammation may also play a role in your heel pain and the health of your plantar fascia, you may want to consider eating a healthy diet that helps minimize chronic, whole-body inflammation. This includes:
- Minimizing common allergens and inflammatory foods, such as processed foods with sugar additives
- Avoiding refined grains, sugar, and alcohol
- Adding more healthy fats, including polyunsaturated fat (e.g. avocados) and omega-3 fatty acids (e.g. salmon and other fatty, cold-water fish)
- Taking supplements that may help to reduce inflammation, such as turmeric
5. Regenerative Therapies
Because of the growing body of evidence pointing to degeneration as a major trigger in the symptoms and causes of plantar fasciitis, you may wish to consider regenerative medicine instead of plantar fasciitis surgery.
Surgery for plantar fasciitis involves cutting the plantar fascia, but this invasive procedure may bring about significant harmful side effects. Risks of surgery include:
- A weak, or even collapsed, arch in your foot
- Reduced function in your foot
- Chronic pain
- Nerve damage
- The need for additional surgery to address these side effects, such as calf muscle surgery
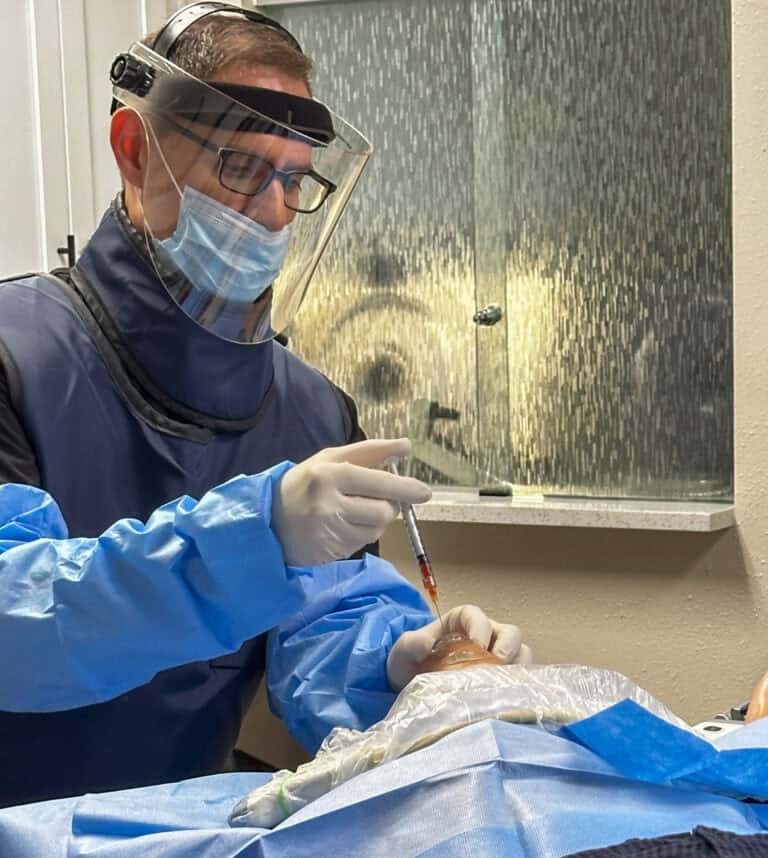
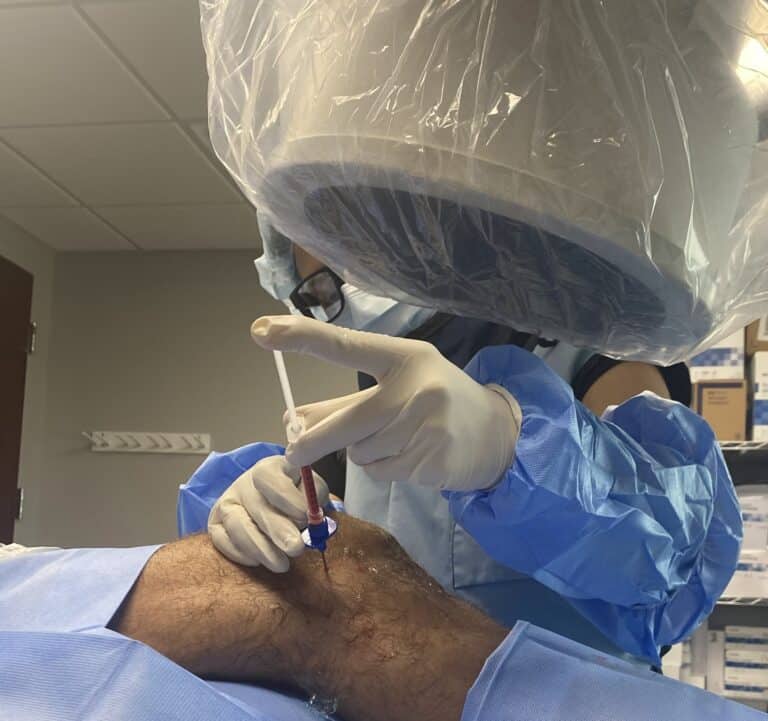
Groundbreaking new research highlights the value of platelet rich plasma (PRP) injections and other regenerative approaches to heel pain. Best of all, rather than covering up the symptoms, regenerative medicine actually deals with the actual underlying degenerative triggers of plantar fasciitis.
The Regenexx family of treatments uses advanced procedures, such as precise image-guided blood platelet injections and orthobiologic (BMC or MFAT) injections, to help improve the health of your plantar fascia and reduce your plantar fasciitis pain. And all without the significant side effects and risks of traditional surgery or steroids.
And unlike steroid injections and similar treatments, the effects are long-lasting. Whether you’ve just been diagnosed with plantar fasciitis, or you’ve been treating it with NSAIDs, corticosteroids, and other conventional approaches with no success, Regenexx may be able to help.
Step into a new, pain-free life today. Contact us to see if regenerative medicine, and Regenexx, is the right approach for your plantar fasciitis. You don’t have to live with heel pain forever.